Did you know ?
We ALL have yeast living on our skin.
Yes, yeast – as in, fungus… Living… on our skin…
You might think this sounds repulsive, and if that’s the case, you’d be surprised to learn that it’’s actually part of our natural AND HEALTHY flora. The native yeasts of the skin are actually HELPFUL and HEALTHFUL in the skin’s immune response and wound repair. On a larger scale, the right amount of these fungi help your body’s immune system do its job.
However, too much of a good thing, isn’t always a good thing… Just like too much fungus isn’t always fun, Gus. (Sorry, Gus, this had to be said.) If you take antibiotics too often or use oral birth control, your body might start to grow too much yeast. Naturally, there are a host of other factors such as diabetes, Sjogren’s Syndrome, HIV infection, chemotherapy, and weakened immune systems, among other contributors which can further contribute to a yeast imbalance.
In fact, when this normal yeast grows out of control on the skin, a person can get a localized skin condition called tinea versicolor. Be assured that the presence of this rash, alone, does not validate or point to any worries of immunocompromise. Most often, certain factors of the skin and surrounding environment such as sebaceous activity and humidity can contribute to the perfect storm which facilitates this imbalance.
How Would I Recognize Tinea Versicolor?
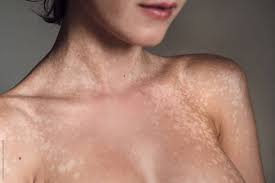
You may recognize the presence of tinea versicolor if you find unusual spots on your skin. These spots may:
-
Appear anywhere on the body (though we typically observe them on the neck, upper back, chest, and shoulders).
-
Cause the affected skin to itch.
-
Appear lighter or darker than surrounding skin; sometimes with a pink, red, white, or brown hue which contrasts the normal skin colour.
-
Feel dry or scaly to the touch.
-
Become more noticeable when you have a tan (because the yeast actually shields the underlying skin from the sun, lightening the skin in contrast).
-
Become less noticeable, even disappearing, when the temperature drops – returning in the spring or summer when the air becomes more humid or your skin begins to tan.
-
Grow slowly, sometimes growing together to form lighter, larger patches.
Is It Dangerous?
While this condition is completely harmless, its appearance and gradual spread is usually disconcerting to patients, especially if the lesions can’t be covered with clothing.
No need to worry; there are a few things you can try following an assured diagnosis from a Board Certified Dermatologist.
Can I Treat It At Home?
First, there are a variety of soaps containing
1) Zinc Pyrithione : Examples include: Vanicream Z-Bar, or DermaZinc Therapy Soap
2) Selenium Sulfide: As found in over the counter Selsun Blue
or
3) Ketoconazole: Prescription strength is 2%; however, over the counter strength is available as ‘Nizoral’ sold in most supermarkets and online.
These can be applied in the shower to wet skin, and left to sit for a few minutes before rinsing off. They work best when used 1-2 times a day for active infection and 2-3 times a month if you have a history of recurrent infections (for maintenance).
Using a net sponge / loofa (no need to scrub aggressively) can help exfoliate the uppermost fungus-infected skin cells and reduce their proliferation. If at-home treatment is performed consistently, improvement should be noted within a couple weeks.
Often, it can be difficult to tell (to the naked, untrained eye) if treatment is successful, initially, as it can take weeks or even months for your skin to return to its usual color. This is because the overlying patches of yeast effectively block the underlying skin from the sun, typically creating a paler skin tone in the effected areas. Wearing sunscreen, UPF clothing, and/or avoiding the sun will help to even out the appearance of tinea versicolor weeks after treatment of the yeast, to give you confidence that this overgrowth is adequately controlled.
What If It Doesn’t Resolve?
Occasionally, over the counter treatments are not enough to stop the growth and appearance of TV. In these cases, lifestyle modifications (looking more closely at clothing, gym gear, bedding hygiene etc) and/or prescription strength oral and topical medications may be recommended by a Board Certified Dermatologist. Intermittent maintenance pulses may also be advised to prevent future growth, especially for those immunocompromised or at risk.
Consider these tips for yourself, or share with a friend who deals with recurrent Tinea Versicolor.
Stay tuned for more helpful insights from Dr. Chaplik and your Aesthetix Team. We believe knowledge is power and information is something you can take with you anywhere. Stay healthy!

